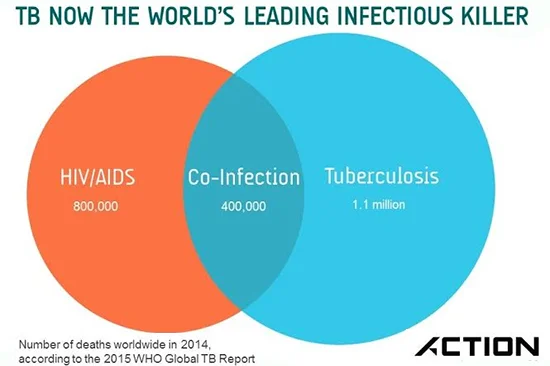
The word's biggest infectious killer
Last week the World Health Organisation published its latest estimates of the TB epidemic. The good news is that the global campaign against HIV has led to a remarkable fall in deaths from AIDS. The bad news is that TB now claims the unwanted title of being the world’s biggest infectious killer. As the Executive Director of the Stop TB Partnership asked:
TB is killing 4,400 people a day and it is now in a shameful leading position among infectious killers. How can we, as human beings accept that a disease that is curable in six months kills more people than HIV/AIDS? What kind of minds and hearts do we have?
1.5 million people died from TB and there were close to 10 million cases last year. These figures come just a month after global leaders agreed the new Sustainable Development Goals (SDGs), which included the target to eliminate TB by 2030. The ambition is laudable. But at the current rate of progress TB won’t be eliminated for another 200 years, let alone 15. The WHO’s plan to end TB currently commands only 75 per cent of the $8 billion a year of global resources it needs. Without a fundamental shift in gear on TB, the SDG target simply will not be achieved. That means millions of lives being lost unnecessarily in the decades ahead - and recurring cost.
Also last week the London Assembly launched the findings of its inquiry into TB in the city. London is already known as the TB capital of Western Europe, but the UK as a whole has surprisingly high rates of the disease for a developed country. There are more cases of TB every year in the UK than there are in Moldova. Parts of the capital have rates equivalent to those in Rwanda and Iraq.
The Government has taken a number of welcome steps to tackle TB. The UK’s pledge of £1 billion to the Global Fund will save a life every three minutes in some of the world’s poorest countries. For the first time in decades (and thanks in part to the work of the APPG Global TB which I co-chair) there is a National Strategy to tackle TB in England. The independent Review of Antimicrobial Resistance, led by Lord (Jim) O’Neill, is looking to include TB in its proposed reforms to incentivise the development of new and much-needed drugs.
But we can and must do more.
First, now that the celebrations over the launch of the SDGs are over, there needs to be an objective appraisal of whether - and how - the programmes currently in place can actually deliver them. The UK is in a great position to do this with the US and other leading donor countries.
Second, meeting the SDG and WHO targets will require greater global political will and more resources to accelerate the reductions in mortality. The Global Fund's fifth replenishment is next year. To date the Fund has supported 13.2 million people to receive TB treatment and saved 17 million lives from the three diseases since 2002. The Fund estimates it will need more than USD$12 billion over the next three years to maintain current progress against the diseases. As one of the leading donors to the Fund since its creation, the UK will have a major role to play.
Third, we need new drugs, diagnostics and vaccines. The current treatment takes six months in a best-case scenario. No new drugs have been added to that basic treatment course for 40 years. The vaccine is ineffective and most diagnoses use technology that’s over 100 years old. No epidemic has ever been beaten through treatment alone - a vaccine has always been needed. If TB had resurged in the West it would have been beaten by now: the pharmaceutical companies would have seen a potential market and had the incentive to invest in new drugs. This is a clear case of market failure. The Conservative Party’s Manifesto included an exciting promise to “… lead a major new global programme to accelerate the development of vaccines and drugs to eliminate the world’s deadliest infectious diseases”. Now we need to hear how the Government will fulfil that pledge.
The Global TB Caucus, an international network of parliamentarians which I set up last year and which currently spans 97 countries, will meet in Cape Town next month. Our aim is to apply pressure to both donor and affected-country governments to ramp up efforts to tackle the disease.
TB is one of the world’s greatest neglected diseases. It also one of the world’s greatest public health threats. It is airborne and infectious, it can become drug-resistant, and it does not respect national boundaries. Lord O’Neill’s team has estimated that 75 million people could die from drug-resistant TB by 2050 if action is not taken.
Already the biggest killer in history, now back as the world’s biggest infectious killer, this is a disease which could beat records again if we don’t act. We can end TB. We just have to decide to do it.